Knowing Your Options with Dry Eye
What is Dry Eye?
Chronic dry eye syndrome is a medical condition more scientifically known as keratitis sicca, or keratoconjunctiitis sicca (KCS) which is Latin for dry inflammation of the cornea and the conjunctiva. It is more a symptom and afflicts one suffering from a dysfunction of the lachrymal or tear gland that produces tears and oil to moisturize the cornea and avoid damage to that part of the eye. If left untreated, dry eyes can result in abrasion to the eye surface that can lead to pathologic changes like squamous metaplasia. Severe cases can thicken the corneal surface or erode, scar and perforate the cornea. It can also result in corneal thinning. In all cases, you can expect both visual impairment and eye discomforts.
Castor oil
Oral secretagogues
Rx Meibomian gland dysfunction
Artificial Tears
Warm Compresses
Punctal Plugs
Steroid eyedrops Moisture Chambers
Punctal cautery
Cyclosporine
Humidifers
Flaxseed oil
Androgen eyedrops
Mucin secretagogues
Note: ![]() identifies 'Experimental' treatment undergoing clinical trials. These are not yet FDA approved for Dry Eye treatment.
identifies 'Experimental' treatment undergoing clinical trials. These are not yet FDA approved for Dry Eye treatment.
Main Causes
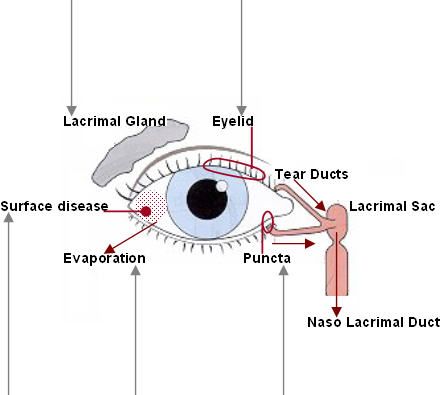
Dry eye is caused by insufficient tear production. There are three layers of tears secreted by the lachrymal gland to produce a stable tear film to protect the outer eye surface. A deficiency or abnormality in any of the layers can result in keratitis sicca or dry eye syndrome. Lachrymal hyposecretion or aqueous tear deficiency (ATD) produces insufficient tears to cover the entire cornea and conjunctiva.
A few ailments cause the symptom like congenital alacrima, sensory denervation, lachrymal glad ablation and blepharitis. The tear glands infiltrated by sarcioidosis, tumors or post radiation fibrosis of the glands can trigger the condition. The condition can also be caused by premature destruction or rapid evaporation of the tears. The medical term is evaporative dry eyes which occur when the lachrymal lands produce inadequate amounts of tears, or the quality of tears is such that it is too saline or hypertonic so that it evaporates faster than normal tears. This becomes acute under certain environmental conditions like extreme cold so that the entire cornea and conjunctiva could not be covered with a layer of tears.
Other Causes
Age is one of the most common culprits in keratitis sicca. It’s a fact the tear gland secretion decreases with age. Post menopausal women are known to suffer dry eyes. The condition is also triggered by accidental chemical splashes to the eye that cause chemical burns. Diabetics are also known to suffer greater risk to the syndrome
Statistically, about 50% of people who wear contact lenses have been documented to complain of dry eyes. Soft contact lenses which float on the tear film covering the corneal surface absorb the tears and that constant use can reduce or damage nerve sensitivities in the cornea that can lead to diminished lachrymal gland tear secretion and thus, result in dry eye syndrome. This causal link between loss of corneal nerve sensitivity and lachrymal production is currently being confirmed in many clinical researches.
Dry eyes also happen after LASIK and other refractive surgeries are performed when they cut the corneal nerves in the creation of corneal flap. Corneal nerves stimulate tear production but such surgeries can cause dry eye syndrome. While in many cases, the condition resolves itself after a few months, the resulting dry eyes can be permanent. This is often the risk in refractive surgery.
Several drugs are also known to cause dry eyes. They include nasal decongestants, antihistamines, oral contraceptives, diuretics, beta blockers, sedatives, anti- hypertensives, trycyclic anti-depressants and pain relieving opiates like morphine.
Dealing with Dry Eye Syndrome
Treating dry eyes is often a matter of avoiding aggravating factors, stimulating tear gland production, rehydration, treating eye inflammation and increasing tear retention.
Dry eyes get aggravated by pollution and dry environments with lots of smoke and dust as well as work places with de-humidifiers and air conditioning. Blinking is a natural process that aids in moisturizing the eyes and should not be deliberately controlled. Too much concentration staring onto computer monitor screens can aggravate dry eyes. Purposely blinking more often and resting tired eyes minimize the condition.
Dry eyes can be rehydrated with eyedrops or artificial tears and some people need this more than others. Artificial tears moisten the eyes but this is a temporary relief that can last for a few hours and cannot stimulate tear gland production. Use autologous serum eye drops since they contain essential tear components like fibronectin, epidermal, neurotrophic and hepatocyte growth factors, and vitamin A which most commercial tear formulations leave out. In addition, lubricating tear ointments that contain white petrolatum and mineral oil is recommended before sleep since they cause blurring – something you will not want during your waking hours.
Medication in the form of mild topical immunosuppressants and steroids is recommended when there’s inflammation due to the tear film’s hypertonicity. Prednisolone and cyclosporine are usually used. In addition, clinical trials have shown that these drugs can stimulate tear gland production in 15% of test subjects.
Recent research shows that consumption of fish containing omega-2 fatty acids can decrease dry eye conditions in women. Early clinical trials points to its efficacies when applied topically.